Here are the treatments for Brugada Syndrome performed by Dr. Stefano Grossi.
Low-Risk Patients
For patients considered low-risk, preventing adverse events involves lifestyle modifications. All patients with Brugada Syndrome should receive a detailed list of medications to avoid (available at www.brugadadrugs.org).
Key recommendations include: Avoid the use of recreational drugs, particularly cocaine, as well as excessive amounts of alcohol and food. Promptly address fever with paracetamol or ice, as elevated temperatures above 37.5°C can inhibit sodium channels and promote arrhythmias.

High-Risk Patients
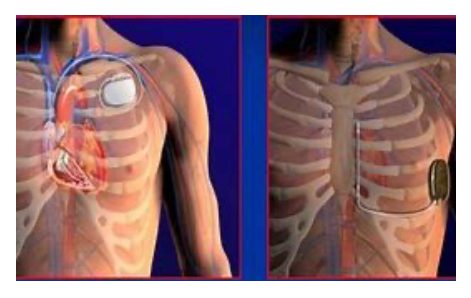
For high-risk patients, including those who have experienced significant events such as syncope with spontaneous Type 1 pattern, aborted cardiac arrest, or documented major spontaneous or induced ventricular arrhythmias during electrophysiological study, the implantation of a defibrillator is recommended. The defibrillator delivers a life-saving electrical shock in the event of severe ventricular arrhythmias (see Fig. 3).
Considerations: While defibrillators prevent sudden death, they can pose challenges, such as: o Painful shocks, sometimes triggered by non-serious arrhythmias. o Malfunctions or infections that may necessitate removal of the device, a procedure with inherent risks. Subcutaneous defibrillators reduce, but do not entirely eliminate, these complications.
Intermediate-Risk Patients
For intermediate-risk patients, pharmacological treatment may be considered. The drug of choice is quinidine, a Class IA antiarrhythmic that blocks potassium channels. Clinical studies demonstrate its efficacy in preventing arrhythmic recurrences in 70–100% of cases. Quinidine Side Effects: Prevalence: Side effects occur in 20–40% of patients. Common Issues: Thrombocytopenia, diarrhea, esophagitis, allergic reactions, QTc prolongation, and torsades de pointes. Discontinuation Rate: About 30% of patients stop the drug due to side effects.
This page describes the standard clinical protocols
(medications, prevention, defibrillator).
If you are looking for an advanced therapeutic solution or want to evaluateAblation as a definitive alternative to medications and the defibrillator:
Treatments
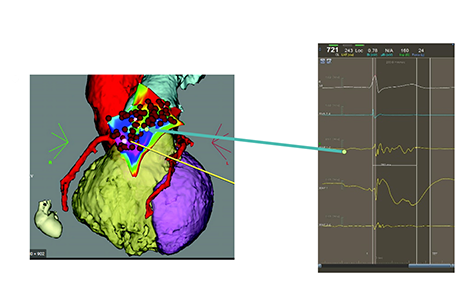
In 2011, electrophysiologist Nadamanee identified a region in the right ventricular outflow tract, located beneath the epicardium, as the source of electrophysiological abnormalities responsible for Brugada Syndrome.
Ablation Procedure:
An ablation catheter is inserted into the pericardium, the protective sac surrounding the heart. The abnormal cells, identifiable by their distinct electrical potentials, are destroyed using radiofrequency energy. This eliminates abnormal electrical signals on the heart’s surface, resolves the Type 1 ECG pattern, and eliminates the arrhythmic substrate. A follow-up electrophysiological study confirms the absence of inducible arrhythmias at the end of the procedure.
This approach is highly effective in the elimination of the electrophysiological substrate of Brugada Syndrome.
For more complex cases, Dr. Grossi performsBrugada Syndrome ablation using robotic technology, a procedure in which he is an international pioneer.
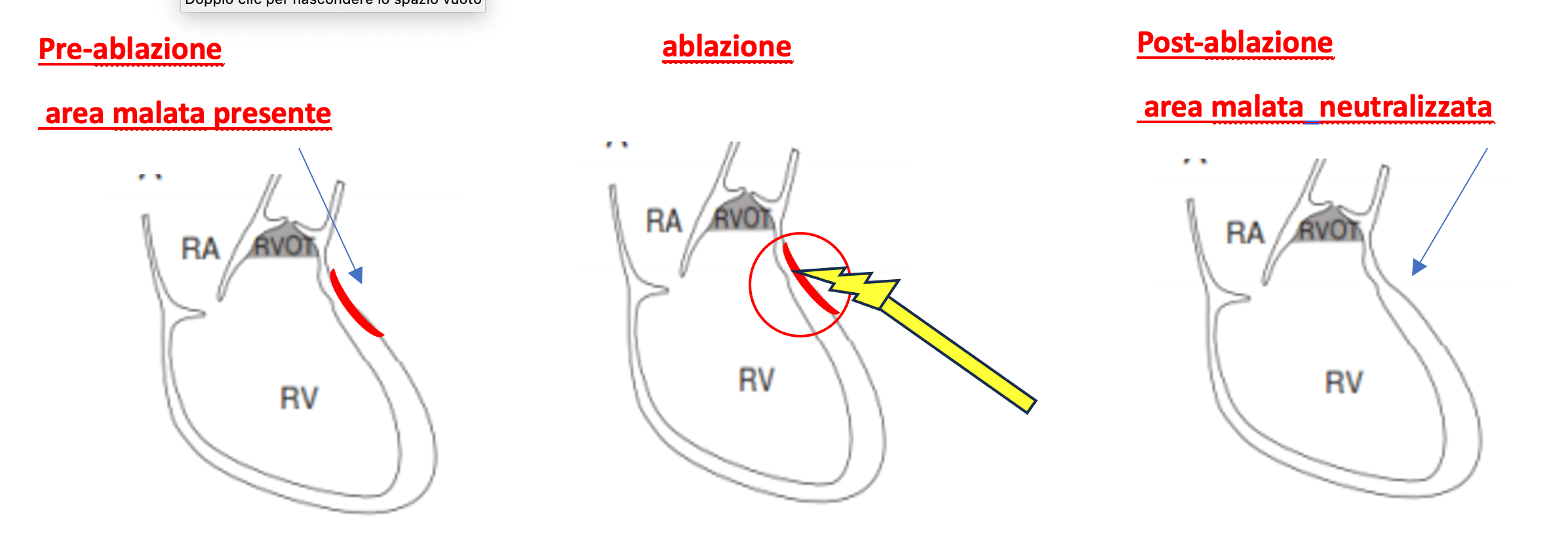
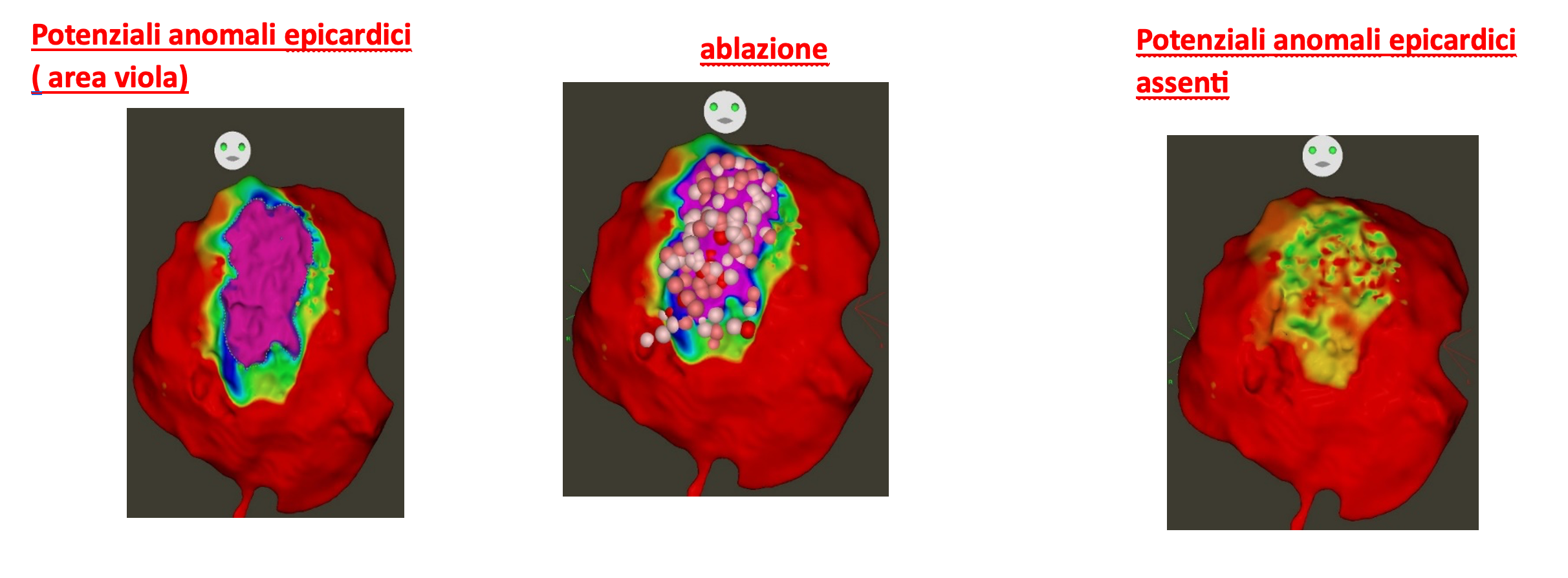
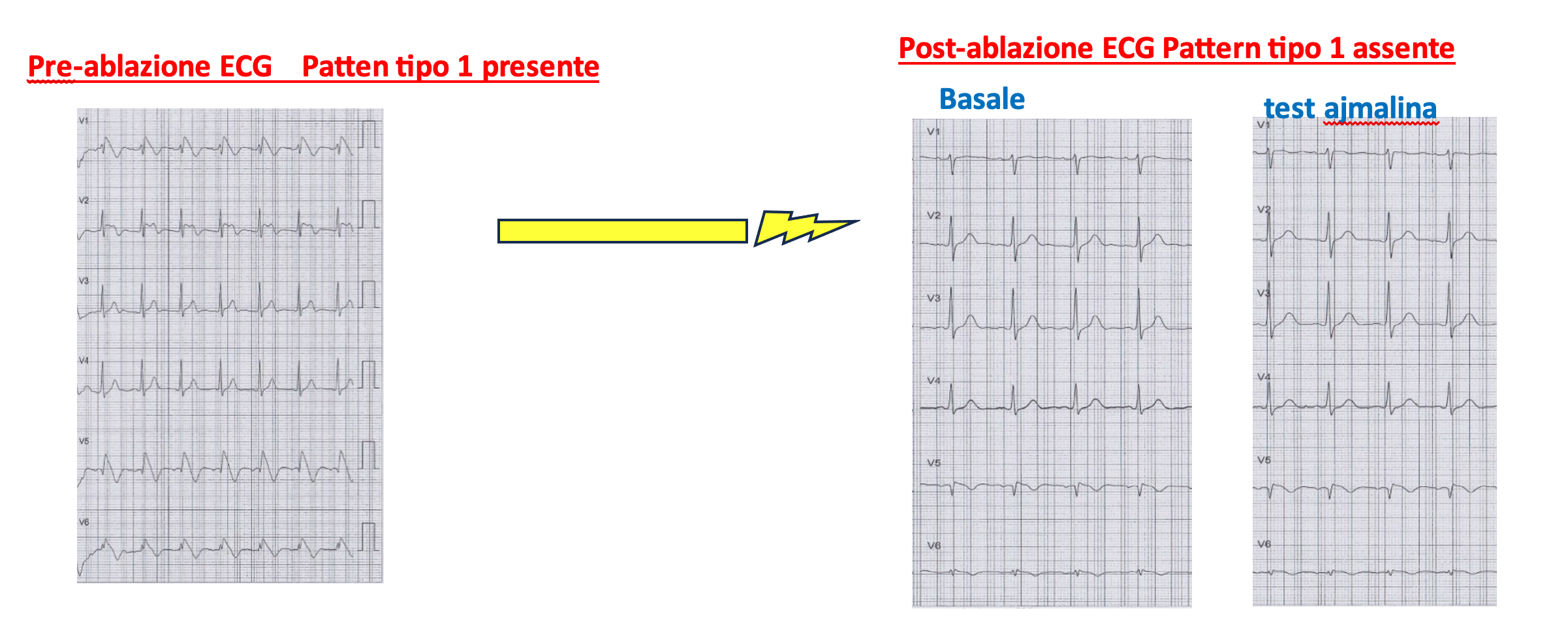
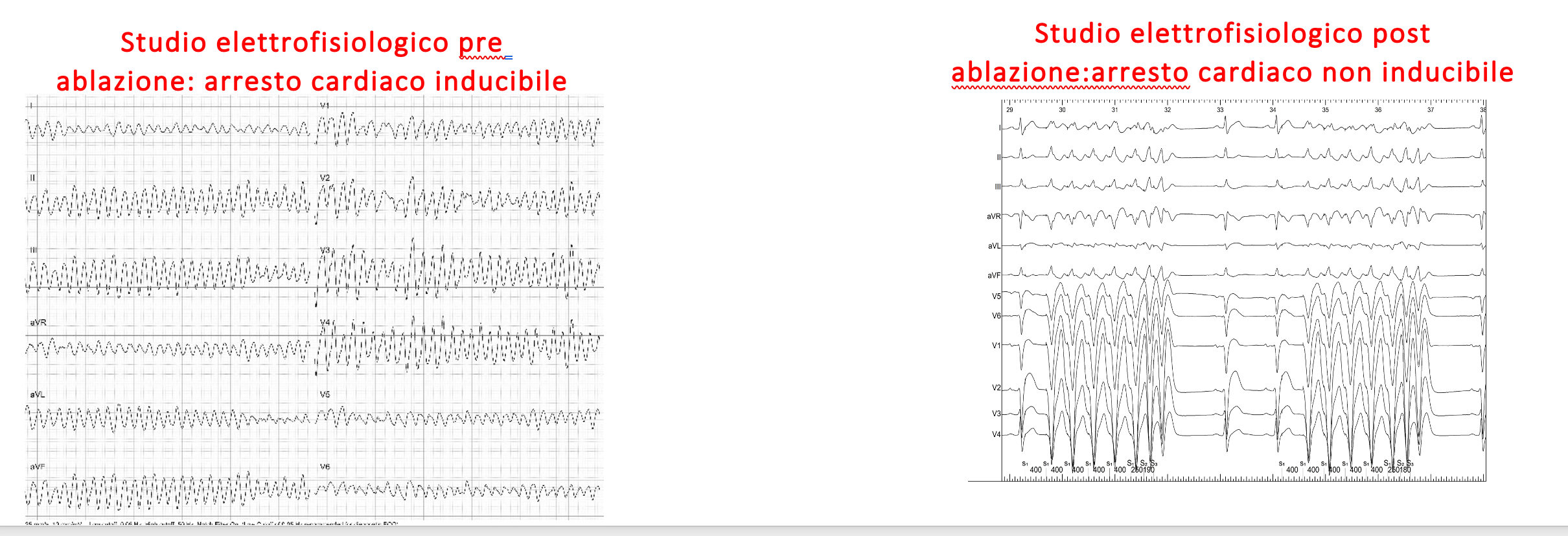
The disappearance of the Type 1 pattern must be evident at the end of the procedure and confirmed after at least one month, both under baseline conditions and with an ajmaline provocative test.
At this point, the ablative treatment can be considered effective.
Numerous studies on ablation for Brugada Syndrome have shown excellent results, with the disappearance of the Type 1 pattern and absence of ventricular arrhythmias in over 80% of cases after the first procedure and in 96% of treated patients, with an intraprocedural complication rate below 2%.
Summary
In summary, for Brugada Syndrome, a defibrillator is deemed necessary for patients at high risk of sudden death. If arrhythmic episodes are frequent, defibrillator interventions can be minimized with quinidine. When quinidine is not tolerated or when lifelong medication is undesirable, ablation—which addresses the arrhythmia's root cause—has shown high efficacy. Collected data will soon clarify whether ablative treatment can be considered effective enough for high-risk patients to avoid defibrillator implantation.
For patients where the risk does not justify a defibrillator due to its potential consequences, certain subgroups may still have a non-negligible risk. Asymptomatic patients with a spontaneous Type 1 pattern have an annual arrhythmic event risk 100 times higher than unaffected individuals. In such cases, ablation can significantly reduce this risk without requiring a defibrillator or continuous medication. The same reasoning applies to asymptomatic patients with a family history of sudden death or inducible arrhythmias during an electrophysiological study. Treatment must always be individualized and discussed collaboratively between doctor and patient, emphasizing an effective doctor-patient alliance.

Il Dott. Stefano Grossi ha eseguito ad oggi più di 200 ablazioni in pazienti affetti da sindrome di Brugada , la sua è a tutt’oggi la seconda casisistica al mondo.
In 2018, he performed, for the first time in Italy, an ablation procedure for Brugada syndrome using the Stereotaxis robotic magnetic navigation system.

