What are the treatments for
atrial fibrillation?
The treatments for atrial fibrillation are divided into two parts: the prevention of thromboembolic events and the treatment of the arrhythmia.
First and foremost, it is essential to effectively address any predisposing conditions: associated heart diseases, hypertension, obesity, metabolic disorders, thyroid dysfunctions, etc.
Stroke prevention (thromboembolic events)
The risk of stroke is not the same for all patients with atrial fibrillation. There are clinical characteristics associated with atrial fibrillation that indicate how likely a patient is to experience a stroke. Each of these clinical characteristics is assigned a score: congestive heart failure (1 point), hypertension (1 point), age ≥ 75 years (2 points), age between 65 and 74 years (1 point), diabetes (1 point), history of stroke/TIA (2 points), history of myocardial infarction, aortic plaques, or peripheral vascular disease (1 point), and female gender (1 point). Patients who score 0 have a very low risk, and thus no antithrombotic prophylaxis is necessary.
Patients with only one point have a still relatively low risk, and treatment must be evaluated on a case-by-case basis by the physician.
When a patient scores two or more points, it is necessary to initiate antithrombotic treatment, as the annual risk of stroke ranges from 2.2% to 15.2%. The recommended treatment involves oral anticoagulant medications, which have been shown to reduce the risk of stroke by approximately 70%. Today, therapy with vitamin K antagonists (such as warfarin or coumadin) is indicated only in the presence of a mechanical heart valve or mitral valve stenosis. In all other cases, New Oral Anticoagulants (NOACs) are used.
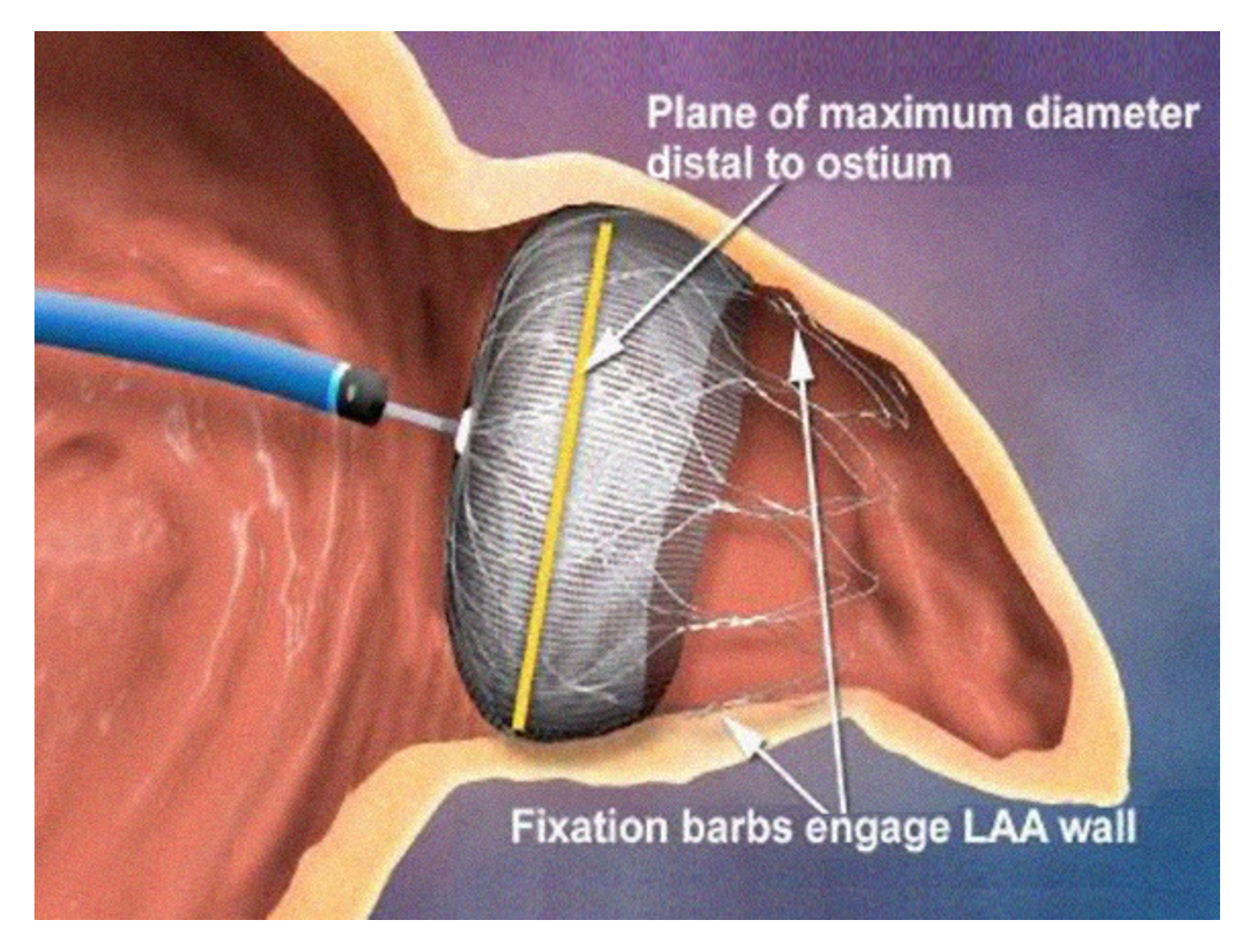
If anticoagulant treatment cannot be administered due to a high risk of bleeding, other intolerances, or proven ineffectiveness, the patient may undergo a left atrial appendage occlusion procedure. This is because 90% of blood clots form within a cavity connected to the left atrium, known as the atrial appendage.
The complete occlusion of this cavity prevents the formation of clots and, consequently, the detachment of fragments (emboli), which, if released into the bloodstream, can cause embolism and stroke.
Treatment of arrhythmia
Restoration of sinus rhythm
The acute onset of atrial fibrillation that is poorly tolerated by the patient represents a cardiac emergency and must be treated in the emergency department. It should be interrupted as soon as possible, if feasible, through electrical cardioversion.
In most cases, although the patient is symptomatic, their condition is not severe and can be assessed more calmly. It is important to note that many episodes of paroxysmal atrial fibrillation resolve on their own.
The physician's primary goal is to restore the normal heart rhythm (sinus rhythm), which can be achieved through electrical or pharmacological cardioversion (administration of an antiarrhythmic drug), depending on the patient's characteristics and the resources available at the healthcare facility. Rhythm restoration can be performed immediately within 24-48 hours of the arrhythmia's onset. After this time frame, blood clots may form in the atrium, and before restoring the rhythm, it is necessary to dissolve them with anticoagulant therapy. Therefore, the treatment will initially focus on slowing the heart rate, and rhythm restoration can only be performed after an appropriate waiting period, typically around three weeks. This waiting period can be shortened if necessary by following a protocol that includes performing a transesophageal echocardiogram to rule out the presence of clots in the heart.
Maintenance of sinus rhythm
Almost all cases of atrial fibrillation can be interrupted. The real challenge in the treatment of atrial fibrillation lies in maintaining sinus rhythm, as atrial fibrillation has an extremely high tendency to recur.
For many years, antiarrhythmic drugs were the only option for maintaining sinus rhythm in patients with atrial fibrillation.
However, their effectiveness for this purpose is limited, as after one year, no more than 20% of patients remain in stable sinus rhythm. The majority of them will have experienced recurrences.
Furthermore, their use is burdened by undesirable side effects, and many of them are contraindicated in the presence of associated structural heart disease.
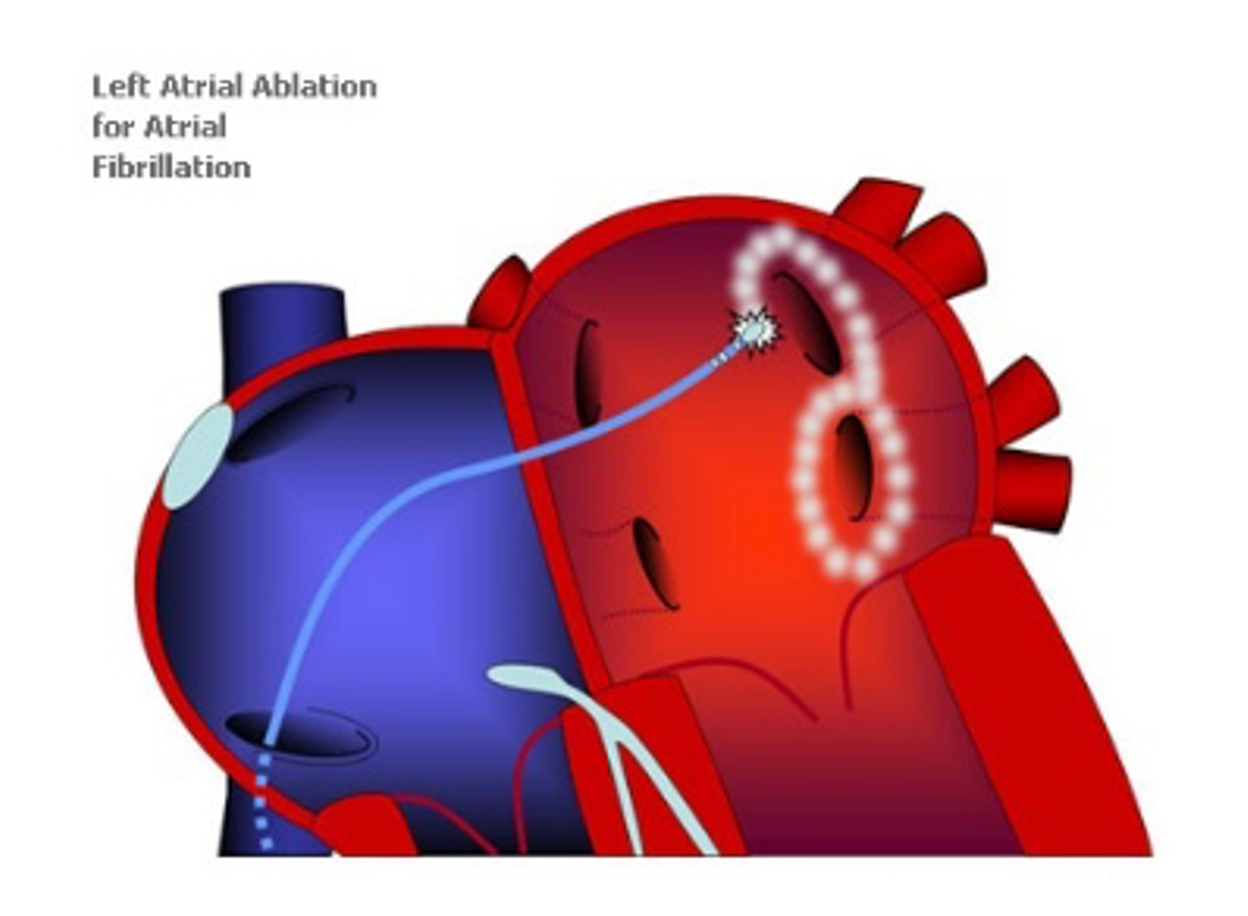
For this reason, in cases of ineffectiveness or intolerance to medications, or when the patient does not wish to take them continuously, cardiology guidelines recommend performing a catheter ablation procedure.
The ablation procedure works by eliminating the altered cardiac cells responsible for triggering and maintaining the arrhythmia.
The effectiveness in maintaining sinus rhythm is far superior to pharmacological treatment. In the paroxysmal form, the least severe, the procedure cures 80% of the treated patients.
In persistent and permanent forms, the success rate gradually decreases depending on how advanced the atrial disease is.
For this reason, the ablation procedure should be performed early in the natural history of atrial fibrillation, when the left atrium has not yet developed extensive disease.
Dr. Stefano Grossi has performed over 5000 atrial fibrillation ablations, adopting all the techniques made available by various technologies.
Thanks to these techniques, even in chronic forms, atrial fibrillation can be eradicated in the long term through one or more procedures.
In July 2022, Dr. Stefano Grossi performed the world's first endo-epicardial atrial fibrillation catheter ablation and left atrial appendage occlusion using the Lariat system with a percutaneous, non-surgical approach.
With this technique, it is possible to achieve good results in treating patients who are refractory to traditional endocardial ablation procedures.
Heart rate control
In patients with long-standing atrial fibrillation, with very advanced atrial disease, who cannot be maintained in rhythm by any means, or in those where further attempts are not pursued due to very advanced age or significant comorbidities, the cardiologist limits the treatment to slowing the heart rate with digitalis, beta-blockers, or calcium antagonists.
Atrial fibrillation will thus become permanent. In the few cases where it is not possible to achieve heart rate slowing with medication, the patient may undergo ablation of the atrioventricular node and simultaneous pacemaker implantation: in this way, atrial fibrillation will remain confined to the atria, and the heart rate will be determined by the pacemaker's settings, as decided by the cardiologist.

